Mamas Uncut’s Scott McClellan sat down (remotely) with Dr. Noah Greenspan, PT, DPT, CCS, EMT-B, a cardiopulmonary rehabilitation specialist in New York City to discuss his experience working with COVID-19 “long haulers.” Dr. Greenspan is the Founder of the Pulmonary Wellness Foundation (PWF), a group of tippy-top experts in their respective fields, that have recently launched a FREE COVID-19 Rehab Bootcamp. The CDC has recently recognized this large and ever-growing group of people in a recent post. Early estimates suggest that roughly one-third of people who have recovered from their initial COVID-19 infection continue to experience serious health issues weeks or months later.
COVID-19 is Not Just a Respiratory Illness
Mamas Uncut: What has been your experience working with COVID-19 patients so far?
Dr. Noah Greenspan: We live in New York City where we obviously got hit very hard, very early. We made the difficult but correct decision to close the Pulmonary Wellness & Rehabilitation Center on March 10th because we saw the writing on the wall and we cannot with a clear conscience ask the oldest sickest patients in New York City to risk coming to the center.” Through the foundation, we started working early on to educate the public and especially those at the greatest risk about prevention of COVID-19. We also tried to learn as much as we could about COVID by seeing COVID patients remotely and to try to create some order out of the chaos. What we did initially was take what we knew about the respiratory system, about the cardiovascular system, because initially, everyone thought this was a respiratory virus that you have to go through for 2 weeks and then it’s back to business as usual..
What we learned very quickly is that not only is it not a respiratory problem, but in many cases, it’s a respiratory problem superimposed on a cardiac problem, superimposed on a neurologic problem, and then there’s this whole other mixed bag of symptoms, with every system adding its own unique contribution to this COVID-19 tapestry.
When you have a situation like COVID-19, that is so chaotic on so many levels, it is crucial that we try to restore some semblance of normalcy in the world, some order out of the chaos, and the way we tried to create order is by listening to people’s stories, trying to collect as much information as we can and by trying to recognize similarities and differences among patients. We were often spending two hours or more during our initial consults with patients, really listening, and looking for anything that would anchor us to some kind of solid base to begin standing on.
At this point we’ve probably seen about 100 or so “long haulers” and little by little, we are starting to see similarities, start to see differences and starting to see a light at the end of the tunnel. One of the most accurate statements that I’ve heard about COVID is by one of my friends and colleagues, Dr. Louis DePalo who said, “Ask me about COVID every week and every week I’m going to give you a different answer.” And that’s really how it feels. It’s like each week, there’s some new buzz. So, this week, it’s respiratory, then it was cardiac, then blood clots and then the buzz was “long hauler.” Now, the buzz is “dysautonomia.”

I think for the majority of long haulers, if they were to present to an emergency department at any other time in history, with these types of symptoms, they definitely would have been admitted to the hospital, and many of them probably would have been admitted to the ICU. Instead, due to the sheer magnitude of the situation with respect to both numbers and severity, we basically had a lot of patients that were sent home to fend for themselves, and really by the grace of G_d, or whatever else it is that you may believe in, they survived. But for many, it was way too close for comfort.
Mamas Uncut: I had never heard of dysautonomia until after I described my own COVID-19 experience to you. Can you provide a quick explanation to those not familiar with it?
Dr. Noah Greenspan: At the most basic level, dysautonomia is how it sounds…dysfunction of the autonomic nervous system. The caveat is that for most people, it is not basic and it can take on many forms from person to person, and even for the same individual from day to day, or sometimes, even hour to hour, or minute to minute. The nervous system is composed of the central nervous system (CNS), aka the brain and the spinal cord and the peripheral nervous system (PNS), which consists of nerves and nervous tissue outside of the brain and spinal cord that send messages to the rest of the body including muscle and organs.
The PNS is further divided into the somatic nervous system (SNS) and the autonomic nervous system (ANS). The autonomic system is the division that is affected by dysautonomia. Are you with me so far?
To further clarify, the CNS carries out sensory, motor and integrative functions. The PNS performs sensory functions, sending messages back to the CNS, which then integrates and acts on this information to maintain homeostasis, or stability within the body. Finally, the ANS is subdivided into the sympathetic nervous system and the parasympathetic nervous system. The SNS is mediated by adrenaline and is excitatory. It is responsible for triggering the “fight, flight or freeze” response. The Parasympathetic nervous system is mediated by acetylcholine and is the “rest, digest, and heal” part of the system.
Dysautonomia can impact all of these components and to simplify, we can have problems with how the messages are transmitted to the ANS, we can have problems with how the ANS receives the messages, we can have problems in how the ANS transmits messages back to the CNS and we can have problems with how the CNS receives, integrates and acts on that information.

Breaking it down one step further, what it boils down to is poor communication and like any relationship, communication is key. As a result, some of the more common symptoms of dysautonomia can include: lightheadedness, dizziness or fainting, vertigo. shortness of breath, fast, slow or irregular heart rates, substantial blood pressure fluctuations, particularly with positional changes, among many others. And essentially, each physiologic system can have its own specific symptoms in the context of dysautonomia.
So, the key to successful rehab is to first ensure that the patient is stable enough to participate in the program safely, and this is where communication with the patients doctors, their PCP, cardiologist, neurologist, pulmonologist, is essential. Once they have determined that there are no red flags with respect to the cardiovascular system, the neurologic system and the respiratory system, then we can begin. In the overwhelming majority of cases, while uncomfortable, the symptoms associated with dysautonomia are not life-threatening and at this point, a substantial part of the therapy includes improving communication between the various components of the nervous system and retraining how the body responds.
We also initiated the COVID Rehab & Recovery Lecture Series, where we started bringing in top physicians and specialists who were seeing a ton of COVID patients, including pulmonologists, cardiologists, neurologists, GI doctors, and it was really like a super postgraduate level course in which we got to share our own experience with patients with the experience of top specialists, compare notes, and little by little, we are starting to get a handle on it, with the key word being “starting.”
Two years ago, PWF created an online cardiopulmonary bootcamp for people with heart and lung disease, so we had a little bit of a head start. We had this program locked and loaded, and naturally, we thought this would be the perfect program for our COVID patients because it was designed to be a very gentle program to be used by older people, and/or by people with severe and in many cases, multiple medical conditions. However, what we found was that in many cases, it was still too vigorous for the COVID patients. So we went back and revamped the whole program. So, instead of starting at four minutes of walking, we started people at one minute and then two minutes, and then three minutes. And again, little by little I think we’re starting to get our arms around how we deliver those rehabilitation interventions.
Mamas Uncut: I think medical professionals such as yourself are doing a lot. I think PCPs are already so overwhelmed by the amount of emails and calls they receive on a regular basis that they do not have time to really dig into all of the emerging data. That creates the issue where there are a lot of people, with no medical background like me, who are just scrambling and looking for answers, and trying to figure out, “How do I get better? How do I get back to work? How do I do all this?” Obviously, we’re looking to professionals like you and specialists since you’re in a much better position to help to figure this out.
Dr. Noah Greenspan: Understood, but we cannot do it without you. That’s why as a healthcare professional, you have to be willing to listen to your patients, and you have to be willing to think, and you can’t assume that you know. COVID is like nothing else that we’ve ever seen before. It’s almost like you say, “Reach your hand into this bag of fortune cookies whatever it says on your fortune, that’s what your day is going to be like and these systems will be affected, and these will be your symptoms.”

COVID-19 Long Hauler Symptoms
Mamas Uncut: A group of people, long haulers, seem to be experiencing long-term adverse side effects for at least weeks or months after contracting the virus. What do we know so far about these patients?
Dr. Noah Greenspan: So I think again, we’re starting to get our arms around it, but I think there is still much more that we don’t know than what we do know. Why do some people cruise through it without even knowing they had it and other people are still struggling with symptoms six or seven months later? Why did some people have a cold-and-flu-like experience, whereas others feel like they got hit by a bus?
Mamas Uncut: What are some of the issues, symptoms, long haulers are having?
Dr. Noah Greenspan: So if you look at the long haulers, and there’s a lot of them, there was this huge grassroots advocacy movement to be recognized. It was like “hey we’re here. Hey, it’s been more than two weeks or two months (or more), and hey, guess what? I feel worse than I did back then.” So initially, the goal was to at least recognize that being a “long hauler” is actually a thing.
Now why is that? My gut feeling, and I have no proof to back this up, but… if you think about it, most long haulers were not hospitalized. So many of these long haulers, went to the hospital or ER, and were told, “Ride it out at home,” or so many of these people that thought about going to the ER were told, “shelter in place. You’ll get through it.”
And again, at any other time in our history… and by that I mean the sheer magnitude of this crisis, in terms of the severity and complexity of a new virus, as well as the numbers, as well as the shortage of supplies and equipment, as well as the crazy geopolitical insanity that went along with this whole thing. I think the majority of these patients probably would have been admitted. I mean, you come to the ER, and you have 103.5 fever, and they send you home, I mean that’s unheard of! “You’re not sick enough.” What do you have to do to get admitted, burst into flames?”
If you’re in the hospital and especially in an ICU, where you are being monitored extremely closely, and something doesn’t feel right, you get worked up and you’re treated for it. So maybe these patients wouldn’t have had these long festering insults to the respiratory system, to the cardiovascular system, to the neurologic system. If you get into a car wreck and nobody finds you for a week or two or twelve, you’re going to have a very different recovery than the person who was immediately rushed to the hospital and treated.
Initially the only people being treated were people whose situations were life and death. If you weren’t going to die in the next 4-5 hours you weren’t admitted to the hospital. A lot of these people got lucky in that they survived, but they got unlucky in that they didn’t necessarily get what they needed from the start. And it’s nobody’s fault. It’s just by the nature of the situation. But I’m hopeful and optimistic that over time these people will get back to where they were, but it’s taking a lot longer than we want
Why Is COVID-19 So Serious for Some?
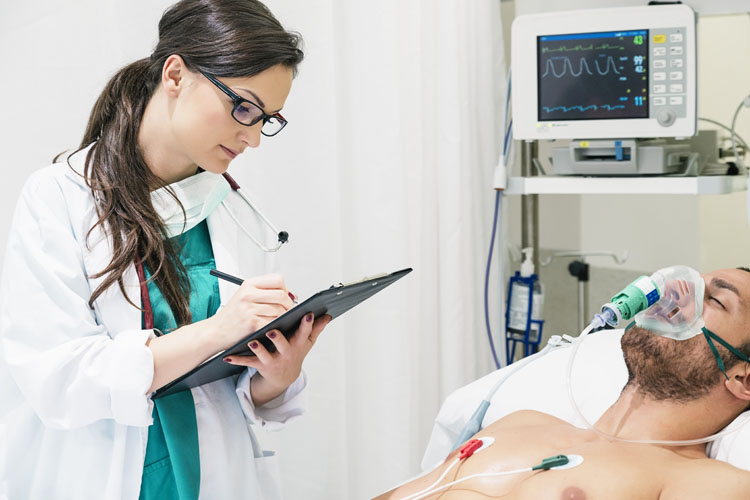
The long haulers I’m seeing are in their 20s, through their 50s or 60s. They’re not people in their 70s, and 80s, and 90s.
Mamas Uncut: Do scientists, doctors, have any inkling so far as to why the virus affects some for so long and in such severe ways versus others?
Dr. Noah Greenspan: So we know that there were certain conditions like advanced age, pre-existing conditions, heart disease, respiratory disease, diabetes, obesity that put us at higher risk. It makes sense that the worse shape you go into something the worse you’re going to come out of it, or the more severely it’s going to hit you. But the one thing I will say is that people from our community; people with chronic heart disease, chronic lung disease, older people, heeded the warnings pretty diligently and they stayed home. We closed our practice and we said to our patients, “stay home.” I was doing daily broadcasts saying, “stay home. I have been saying, “wear a mask,” since day one.
The people at higher risk took it seriously, but other people felt like they had more leeway. To answer your question, it really runs the gamut. There are people, who you would think would be at high risk, that didn’t catch it. There are people who you would think would be high risk that got it and pulled through it. There are people who you wouldn’t necessarily think would be high risk but they got it and it was severe. And there are people who were healthy and fit, that got it and died. I know people in every single one of those categories, so I think that we could say, “Yeah, in theory if you’re older, or if you have preexisting conditions,” but in practice, The majority of long haulers I’m seeing are in their 20s, through their 50s or 60s. They’re not people in their 70s, and 80s, and 90s.
For the people that know COVID, either from personal experience, or who’ve lost somebody, or who somebody they know has gotten sick, they take it damn seriously because it is no joke.
The other day I went to get gas at this place in Southampton, where there’s a sign saying that you have to wear a mask to go inside. I went inside and none of the people that worked there were wearing masks. I asked, “You guys don’t wear masks?” They said, “We do.” I was incredulous, like, “is it invisible?” They said “sometimes we do.”
This was a moment of clarity for me because there are two types of people in this pandemic. There are those that know COVID and there those who don’t know COVID. For the people who don’t know COVID, it’s either a hoax, or it’s a flu, or they’ll get over it, or it’s not going to happen to them, etcetera, etcetera, etcetera, But for the people that know COVID, either from personal experience, or who’ve lost somebody, or who have a loved one that has gotten sick, they take it damn seriously because they know damn well that COVID is no joke.
So that’s a long roundabout answer to, “Do we know why?” I don’t know why. And certainly it makes sense that if 10 people with COPD are exposed to COVID then they’re probably going to have a worse course than somebody that doesn’t have COPD. But, I’ve seen every combination of who should get it and how bad should it be, and who should make it out alive, and I’ve seen things that totally defy that logic.
Shortness of Breath and Breathing Techniques
I recommend that people try these things and practice them when they’re not in distress. You don’t want to learn how to swim after the ship gets wrecked. So the more you practice them the better it’s going to be.
Mamas Uncut: Any recommendations, breathing techniques, for those who have or think they might have COVID and are suffering respiratory issues?
Dr. Noah Greenspan: Try to take slower, deeper breaths. When people are in distress they breathe fast and shallow, and that increases anxiety, and anxiety makes you more short of breath. So it’s quieting the breathing. In through your nose, out gently through your mouth. But what I would really recommend is to… And I don’t say this as a plug, because we’re not selling anything, but I do say go to our website and register for bootcamp. because the stuff is up there and it works.
Mamas Uncut: What should someone who is experiencing shortness of breath or similar respiratory issues do, regardless of whether or not they have COVID?
Dr. Noah Greenspan: In New York City the most common things I hear people complain about are walking up the subway stairs, walking up a hill, running for the bus. That’s what I call the New York City Pulmonary Triathlon. So the first thing is they need to stop whatever activity they’re doing. Activity is based on supply and demand. The more vigorous the activity, the greater the demand for air and oxygen. So we need to lower the demand by stopping or lowering the intensity of the activity.
There are also positions that you can use that will give you the greatest chance of catching your breath, things like leaning forward on your upper body, like fixing your upper extremities by putting your hands down, or resting on your elbows on a table or by leaning forward with your hands on your knees. What this does is allows the abdominal contents to drop down, clearing the way for the diaphragm and that, essentially, improves respiratory mechanics. So we’ve already cut the demand, now we’re increasing the supply. Then the next thing you do is, instead of trying to take that first breath in, is to exhale and then to just kind of slow the breathing down. It takes practice and I recommend that people try these things and practice them when they’re not in distress. You don’t want to learn how to swim after the ship gets wrecked and the more you practice them the more effective they will be when you need them..

Mamas Uncut: What about people who are short of breath at rest?
Dr. Noah Greenspan: For people who are short of breath at rest, the question is why are they short of breath? For any symptom that you’re going to name, before we apply any intervention, we have to check it out to make sure that activity is safe. A lot of people are experiencing what we refer to as non-specific symptoms, like shortness of breath, chest pain or pressure, lightheadedness. These things can be cardiovascular in nature, they can be respiratory in nature, they could be neurological in nature. So before you begin any new intervention, we have to make sure that it’s not something dangerous.
So if you’re having a real cardiac issue see a cardiologist. Then it’s the brain, then it’s the respiratory system. But tons of people are short of breath and tons of people are complaining of different respiratory symptoms and their chest x-ray is clear, so the question is well why is that? Again, if your PCP is willing to order you a CT scan or a pulmonary function test, you’re collecting the data that can help decide if you need to see a pulmonary specialist or not. If it’s neuro we want to make sure you didn’t have a stroke or are not at risk for a stroke. The key is to really make sure that nothing is getting missed.
Protecting Ourselves and Loved Ones from COVID-19
Mamas Uncut: Aside from hand washing, social distancing, and wearing a mask do you have any other advice, as far as not contracting the virus?
Dr. Noah Greenspan: Simple advice? Don’t be an a**h***. I mean that’s the simplest. It’s so simple. We know how to minimize the risk. We know masks work. We know that social distancing and avoiding crowded places works. We know frequent hand washing works, right? But for some reason, people are making conscious decisions to not take these simple precautions.
Mamas Uncut: There seems to be a difference in the disease when contracted by a young child versus an older adult, any insight?
Dr. Noah Greenspan: I don’t.. I think it’s really unknown why children are not as symptomatic as adults. But again, some children are symptomatic, and some children have died. And it’s easy to point at the statistics and focus on the low percentages as compared to adults. But I can tell you one thing, if it happens to your child, your life will never be the same.
Back to School?

Mamas Uncut: What do you think about schools reopening this Fall?
Dr. Noah Greenspan: If I had a child I would not be sending them to school. It’s that simple. I have one sister who is a teacher and my other sister is a school social worker. I am really hoping that they won’t go back to in-person learning until we have a handle on this. As bad as this has been, and trust me, it’s been horrific, if the numbers start to rise in children, which they already are…it will get a lot worse.
Mamas Uncut: Do you have any advice for family members of long haulers or other COVID-19 patients who either need to care for their sick relative, or who simply want and need advice in the way that they can help or support?
Dr. Noah Greenspan: Number one, go easy. That’s the one thing I would say. Go easy on them because they are already going through a lot. Try to be supportive but not suffocating, not helicoptering. A couple weeks ago, I woke up with an epiphany and I said, ” We know there’s long haulers, we know it’s a thing, but we have to now start to take steps forward and to move out of the darkness into the light again.” So be positive, be supportive without being too overbearing, and protect yourself, and sometimes just listen and be there for them.
It’s a hugely isolating time. physically, socially, emotionally, spiritually, psychologically-so anything you can do to close that gap is a plus.
Advice to COVID-19 Long Haulers

Mamas Uncut: What is your advice for long haulers?
Dr. Noah Greenspan: My advice to long haulers, again, is to go easy. Number one, pick your battles. So understand that we know you’re there, we see you and we’re with you. A lot of long haulers have this idea that somehow they’re being gaslit by their doctors or by the medical community. I can assure you that no doctor is gaslighting any long hauler. Get educated without going bananas. Make sure you’re getting your rest and resting doesn’t mean watching TV or being on Facebook all day, right? Because those things can be inflammatory. When it comes to COVID recovery, the emotional and the physical are intimately interconnected. I would say number one is to be kind to yourself, be gentle to yourself, have faith that this is going to get better and the more patients I see the more I do believe it’s going to get better. And the physicians that we’ve had as our guests are also reiterating that same gut feeling.
COVID is like your house was flooded with sea water and until that water, which represents the inflammation, recedes a little, there’s only going to be so much that you can do. You are only going to heal as quickly as your slowest system and the neurological system is one of the slower systems to heal. You can’t fight it, so listen to your body. Also trust that your body is resilient and is working behind the scenes to help you. It doesn’t mean don’t do anything but it means take it slower than you think you should. Throw the stone or pebble, let the pool ripple, and then based upon that, you move forward.. And do COVID bootcamp!
Mamas Uncut: After finding a support group, I was incredibly relieved, but then found that people are generally posting on their worst days, which is incredibly anxiety inducing. People who have been sick longer than I have which made me doubt my own recovery.
Dr. Noah Greenspan: Yeah, absolutely. You have an emotional, physical and physiologic response to that stimulation. These factors alone can increase the activity of the sympathetic nervous system and this can prevent your body from doing what it needs to do for healing and recovery.
Every day that goes by I feel more confident in the ability of long haulers to heal. A lot of it has to do with resisting your natural urges. By that, I mean resist the urge to read 27 studies in one night. Resist the urge to go on Facebook and post this story in 27 groups, and then check every comment. Resist the urge to push yourself beyond your limits. Again, be patient with yourself and your body. This is not the time to be cavalier. This is a time for humility in the face of something that would be difficult for anyone to deal with, and do your best to handle it with grace, and with patience and with positivity. You can get through this!
For Healthcare Professionals

Mamas Uncut: Is there anything you would like to say to the doctors, nurses and other front line workers?
Dr. Noah Greenspan: First and foremost THANK YOU! And I am so sorry that you had to go through this and experience things that no human being should, especially people that are so caring and so sensitive and tuned in to the needs of others. I want to say that you are not alone… and that we see you… and that we are here for you. And I want to say that we are proud of you and that doesn’t just include doctors and nurses, that includes every individual from the first responders to the grocery workers and delivery people and each and every person that continued showing up to work each and every day at great risk to themselves and their families, so that the rest of us can stay safe.
Final Thoughts
Mamas Uncut: Any final thoughts?
Dr. Noah Greenspan: Yeah. Wear a mask,maintain social distance, wash your hands and don’t be an asshole.
Dr. Noah Greenspan, DPT, CCS, EMT-B is a Board-Certified Clinical Specialist in Cardiovascular and Pulmonary Physical Therapy with almost thirty years of cardiopulmonary physical therapy and rehabilitation experience.

Dr. Greenspan began his professional career at the New York University (now Langone) Medical Center’s Rusk Institute of Rehabilitation Medicine, with clinical rotations in medical, surgical, orthopedic and neurologic rehabilitation, chest physical therapy and ultimately cardiovascular and pulmonary rehabilitation. From 1995-1999, he served as the chief physical therapist of the Cardiac Prevention and Rehabilitation Center under the direction of Physiatrist, Horacio Pineda, MD and Cardiologist, Mariano Rey, MD.
In 1998, he founded the Pulmonary Wellness & Rehabilitation Center, a Manhattan-based physical therapy practice specializing in the care of patients with cardiovascular and pulmonary diseases and New York Wellness, a comprehensive outpatient physical therapy practice with orthopedic, cardiovascular and pulmonary, complex medical and airway clearance units. Under his direction, the Center has conducted over 100,000 exercise sessions and been named “Best of the United States” in the area of cardiovascular and pulmonary physical therapy.
In 2014, he founded the Pulmonary Wellness Research and Education Society (renamed the Pulmonary Wellness Foundation) with the objective of coupling excellence in respiratory care with educational material of the highest caliber, delivered free of charge to patients, their family members, caregivers and clinicians, and to support new research projects aimed at better understanding the impact of cardiopulmonary rehabilitation and lifestyle change on safety, efficacy, lung function and quality of life in people living with pulmonary diseases.
In 2017, Dr. Greenspan’s “Ultimate Pulmonary Wellness” was published and is also available to read online free of charge and his “Ultimate Pulmonary Wellness” Lecture & Webinar Series is also available to attend online. He is the principal investigator in three ongoing research projects: The Impact of High Intensity Exercise on Pulmonary Function in Patients with Chronic Obstructive Pulmonary Disease (COPD); The Impact of High Intensity Exercise on Pulmonary Function in Patients with Idiopathic Pulmonary Fibrosis (IPF); and Safety and Efficacy of Cardiopulmonary Rehabilitation in Patients with Pulmonary Hypertension (PH).
A consummate educator, Dr. Greenspan has trained thousands of patients and hundreds of students and clinicians. From 1995-2003, he was on the faculty of New York University, during which time he was awarded the title of Master Clinician in the area of cardiovascular and pulmonary physical therapy. He has since taught at Dominican College, New York Medical College, and Long Island University in the areas of Cardiovascular and Pulmonary Pathology, Diagnosis and Management. He has previously served as the Pulmonary Rehabilitation Fellowship Coordinator for St. Vincent’s Medical Center and the Weill Cornell Medical College.
Dr. Greenspan has served as the Federal Affairs Liaison representing the Cardiovascular and Pulmonary Section of the American Physical Therapy Association and on the Leadership Board of the American Lung Association of the Northeast. In addition to his role at the Center, Dr. Noah Greenspan is a New York State Emergency Medical Technician (EMT) and Advanced Cardiac Life Support Provider; a professional SCUBA Diving International Open Water Instructor, and underwater naturalist, with a passion for shark photography; a musician, artist and clothing designer under the moniker, Noah G Pop!
Dr. Noah Greenspan, DPT, CCS, EMT-B is a Board-Certified Clinical Specialist in Cardiovascular and Pulmonary Physical Therapy with almost thirty years of cardiopulmonary physical therapy and rehabilitation experience.
In 1998, he founded the Pulmonary Wellness & Rehabilitation Center, a Manhattan-based physical therapy practice specializing in the care of patients with cardiovascular, pulmonary and complex medical conditions. Under his direction, the Center has conducted over 10,000 exercise sessions and been named “Best of the United States” in the area of cardiovascular and pulmonary physical therapy.
